‘I can with all confidence say that most days, those of us who are chronically ill certainly feel like we are’
PROVIDENCE- Employees with chronic health conditions are becoming more in the workplace, health experts say. Those with preventable chronic illnesses are also prevalent. Preventable chronic conditions include high blood pressure, Type 2 diabetes, smoking, obesity, and physical inactivity. Chronic health conditions include Type 1 diabetes, fibromyalgia, cerebral palsy and other non-preventable conditions that fall under the category of functional.
These conditions are contributing to the expenses of employers, not only in the form of increased insurance premiums, but also in the form of productivity. Work stress, home stress and pre-existing health conditions all contribute to workforce expenses. On average, Americans who work full time will spend about one-third of their day at their workplace.
Title 42, chapter 87 of Rhode Island law defines disability as “a physical or mental impairment that substantially limits one or more of the major life activities of such individual.”
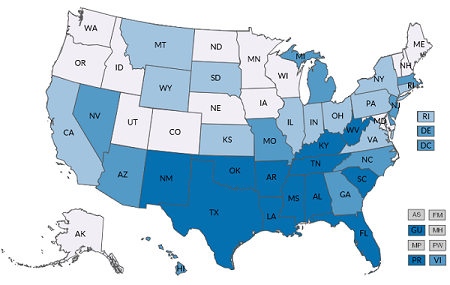
According to the CDC, 222,454 adults in Rhode Island have a disability, about 25% of the total population. This figure is for those who have a documented disability and does not include those who are actively seeking a diagnosis.
The most common type of functional disability, making up 13% of all disabilities, is related to cognition, according to experts. This means that the disabled person has a serious difficulty with concentration, remembering things, and/or making decisions. The next most common disability, compromising 10% of those with disabilities, is mobility. A mobility disability is defined as serious difficulty with walking or climbing stairs. The least common functional form of disability is self-care, a form of disability in which there is difficulty with dressing and/or bathing. These statistics, combined with the percentages of those with hearing, visual and independent living disabilities, compromise 42% of all documented disabilities in Rhode Island.
A 2021 report from the CDC’s Behavior Risk Factor Surveillance System, or BRFSS, conducted in Rhode Island showed that adults with disabilities are twice as likely to be obese, smoke, have diabetes or have heart disease. People with disabilities are three times more likely to have depression in comparison to those without disabilities.
According to Cali McAtee, an epidemiologist with the Rhode Island Department of Health, BRFSS data from 2021 shows that among those with at least one chronic condition, 49.77% are either employed in a wage position or are self-employed; about 17% are out of work or are unable to work and 26.4% are retired. Almost 4% of chronically ill people are students, while another 3% are homemakers. The percentage of adults who are students who also have chronic conditions is just under 4%.
The data shows that many chronically ill people still participate in day-to-day life and encounter many people during day-to-day routines who are chronically ill and may not even be aware of it.
The data from 2022, also provided by McAtee, shows very little change. The percentage of those employed for wages or who are self-employed fell to 48.04% and the number of adult students rose to 5.9%, with the other statistics showing very little deviation. This population sample was also further assessed as to what chronic conditions they have.
It was reported that 35% of employed people were told by a healthcare professional that they have some form of arthritis, rheumatoid arthritis, gout, lupus or fibromyalgia. Also responding “yes” to this question were 20% of those out of work or unable to work and 41% of retired people.
When asked if they were ever told they had asthma, 56%of employed people responded “yes.” Those out of or unable to work compromised about 19%.
About 55% of retired people reported that they had skin cancer, melanoma, or another form of cancer. Just under 31% of those employed for wages or who are self-employed reported a cancer diagnosis.
When asked if they had ever been told they had a depressive disorder, which includes depression, major depression, dysthymia, or minor depression, 48% of those employed for wages or who are self-employed responded “yes.” About 24% of people who are out of work or are unable to work report a depression diagnosis as well. Almost 15% of retired people also have a form of depression.
About 39% of retired adults reported that they are diabetic. . Just under 35% of those employed for wages or are self-employed reported this as well. Among those who are out of work or are unable to work, just under 22% are diabetic as well.
It is important to note that the respondents have only been told that they have these chronic conditions. These conditions may not be the reason why the respondents are medically disabled. Based on these survey questions, it is impossible to know, as these questions only show part of the story.

However, there are a few conclusions that can be drawn from this data. First, chronic illness affects many individuals. There are quite a few individuals who are still employed in some way, though the data does not differentiate between part-time and full-time work, and this sample population has the highest rates of asthma and depression. Also shown in the data is that the retired population has the highest rates of diabetes, physical pains, and cancer. But the data presented here does not show the toll chronic illnesses take on caregivers or on the economy, which can be considerable.
While the data analysis for 2023 is not yet completed, there is a possibility of further deviations, especially when it comes to the percentage of people employed, those out of work, and those retired. Depending on other healthcare data, such as hospital and primary physician reports, the Department of Health may also choose to focus on other chronic conditions, such as heart health, in addition to their established baseline data.
It is estimated that the state of Rhode Island spends about $3.7 billion per year on health care alone. Once the numbers are crunched, this equals out to about $20,174 per year per disabled person. This represents about 38% of the state’s total healthcare spending. These figures are based solely on the state’s reports of those who have insurance plans and do not include those who have private, or employer sponsored insurance. State insurance plans include plans that can be purchased through the insurance marketplace with plans from Neighborhood Health Plan of Rhode Island, United Health, Blue Cross Blue Shield of Rhode Island, Medicare and Medicaid.
Those individuals who are physically disabled have a few options available to them. If the disability was obtained on the job, then the individual can file for workmen’s compensation benefits. Individuals can also apply for Temporary Disability Insurance, if the disability is deemed temporary by a doctor. The Family Medical Leave Act, or FMLA, will allow an individual to take up to three months of time off for temporary disabilities, such as minor surgeries and recovery periods, among other benefits. An individual can also seek permanent disability status through their doctor, which will allow for the individual to apply for other government assistance programs, such as disability assistance, SNAP and utility assistance.
No matter which option an individual chooses, this process can be detrimental to income. A person who was not born with a disability may find this process causes a significant decrease in income. There is the loss of income from not being able to work, as well as an additional income gap while waiting for benefits to “kick in.” Other expenses may come into play as well, such as if a lawyer is hired to help apply for benefits or help with workmen’s compensation cases. Depending on the size of the disabled person’s family, it may not be feasible for them to not work. From here, the options are narrowed down to two: go back into the workforce or stay home.
The option to go back to work can be disturbing to some people. What if something happens at work? What if my job description is unobtainable? What if my condition worsens? What will my boss and coworkers think of me? Is it possible for me to hide my disability? Do I even tell my boss about my disability?
Individuals with physical disabilities that are not as obvious, such as fibromyalgia and severe hearing loss, may face harsher judgement from their peers for simply not appearing to be disabled. Disabled people may feel that they must work twice as hard to prove themselves to their boss and coworkers. In doing do, they push themselves to their physical limit, which can cause their disability to flair up or for new symptoms to arise, thus continuing the cycle of illness, time off and recovery.
In theory, remote jobs would go easier on the body, allowing for individualized schedules to work around most any situation. Depending on the company, online meetings may be necessary. This type of work provides a way to hide disabilities. Zoom filters allow for the use of different filters for backgrounds, including blurring. Remote jobs, however, are not as popular as they were during the COVID-19 pandemic and many employers requested their employees return to the office, at least part of the time, despite data from the National Institutes of Health, suggesting that productivity during this time did not significantly change. Familial stress, environmental stress, distractions, and other environmental factors often lead to slight negative outcomes of productivity.
A personal experience

Keeping all of this in mind, one could argue that chronic illnesses are a burden to society. Having a chronic illness myself, I can with all confidence say that most days, those of us who are chronically ill certainly feel like we are.
I am part of the 48% of Rhode Island adults with a chronic condition and I am part of the 35% with a physically painful condition. I am employed, full-time, as a nursing assistant and I have fibromyalgia. I am also diabetic, but my diabetes takes a backburner to my fibromyalgia. I am also in school full time, seeking a second degree in nursing.
My job is physically demanding and so are my clinical rotations for school. While I don’t have a problem with this — I signed up for both my job and my schooling—my body does have a severe problem with this.
I like to explain fibromyalgia as just a misfiring of nerves: My brain does not know when to stop sending nerve impulses. It is far more complicated than that, as there are numerous symptoms that I experience, but the important take away from this explanation is that I am in constant pain. There are times when I need to use an arm crutch to walk due to leg pain, which also causes me to lose my balance. There are times when I injure myself more while trying to meet basic needs. For example, I have broken my foot due to shooting nerve pains that have caused me to trip and fall.
My symptoms are varied and confusing. They include fatigue, an intolerance to both extreme heat and cold and the ability to predict the weather better than any weatherman in New England, fast heart rates, poor balance, and general malaise, just to name a few. My symptoms can mirror those of multiple sclerosis. They have left both my doctors and I confused, as well as myself on many home heart monitors, trying to figure out if I have other conditions as well. My immune system is compromised, so the tiniest exposure to anything could very well land me in the hospital. It is difficult to determine symptoms from potential illness.
I believe that my insurance company has paid a small fortune for my care, though I cannot be certain of the amount. I can never be sure if I am in “real” pain or if one of my symptoms are flaring up. The pain alone affects my work. I will always put my patients first and take care of them to the best of my ability, but that often means that I ignore my pain and what my body tries to tell me.
This will not be sustainable for me or my company in the long run and truth be told, even after obtaining my next degree, I am not sure how much more I can physically take.






